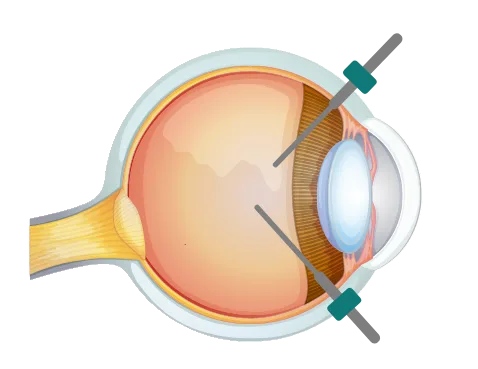
The middle of your eye is filled with vitreous, a clear, jelly-like substance. It keeps the eye in shape. Floaters are common and due to the natural jelly in the eye breaking down with age. A posterior vitreous detachment (PVD) occurs when the vitreous separates from the retina. It occurs in patients over 50, but can occur earlier in patients with high myopia (shortsightedness). The most common symptoms include floaters and short bursts of flashes of lights. However, the symptoms of PVD are similar to retinal detachment which is a much more serious condition, and needs to be excluded. In the vast majority, the floaters usually become less noticeable with time. Dr Bhikoo can discuss and treat persistent and bothersome floaters.
A retinal detachment can cause permanent vision loss if not treated promptly. It is a condition that occurs when the retina detaches from the back of the eye. The symptoms include the sudden appearance of floaters in your vision, flashes of light, sudden blurriness, or the appearance of a shadow moving across your vision. Surgery is often the recommended treatment for retinal detachment including vitrectomy (see below) and/or scleral buckle.
Vitreomacular traction is where the vitreous doesn’t fully detach from the macula at the time of a PVD (Posterior Vitreous Detachment). Persistent pulling or traction on the macula, the part of the eye responsible for central vision, can lead to distortion and/or partial vision loss.
Macular holes arise from vitreomacular traction (above) where the vitreous creates a gap in the macula causing painless loss of central vision. In order to close the hole and improve vision, surgery must be performed in a timely manner.
Epiretinal membrane is thought to affect over 7% of people over the age of 60, and is characterised by a thin film of scar tissue that deposits on the macula/retina. In the majority of cases the condition remains stable, however progressive contraction of the scar tissue can distort the macula leading to differences in image size between the eyes, blurry or distorted vision. Surgery is often recommended in symptomatic individuals or to prevent further macula injury.
A vitrectomy is used to treat a number of vitreoretinal conditions, including all of those listed above. Local anaesthesia and intravenous sedation provide a more comfortable, painless experience. The surgery involves removing the vitreous jelly (floaters) using three tiny key holes, each less than 0.5mm in diameter. Other procedures are then performed depending on the indication, such as retinal detachment repair or epiretinal membrane peeling. At the end of surgery, you’ll have a tiny or large gas bubble in your eye that can stick around for a few days or weeks. You should avoid high altitude travel or scuba diving until the gas has fully dissolved. As the gas dissolves, the eye fills the vitreous cavity up with its own saline solution. There may be a need for you to lie in a certain position for a couple of days after surgery if you have retinal detachment or a macular hole. Dr Bhikoo will explain this to you. Sutures are usually not required and there is minimal pain after surgery, although your eye might look red for a few days. Vitrectomy surgery is generally safe, however like any surgical procedure there are risks which Dr Bhikoo is happy to discuss with you during the consultation. He has performed thousands of retinal procedures and surgeries. He uses the latest techniques and technologies to hasten recovery and enable quick return to function following surgery.